
by Stemedix | Aug 23, 2021 | Stem Cell Therapy
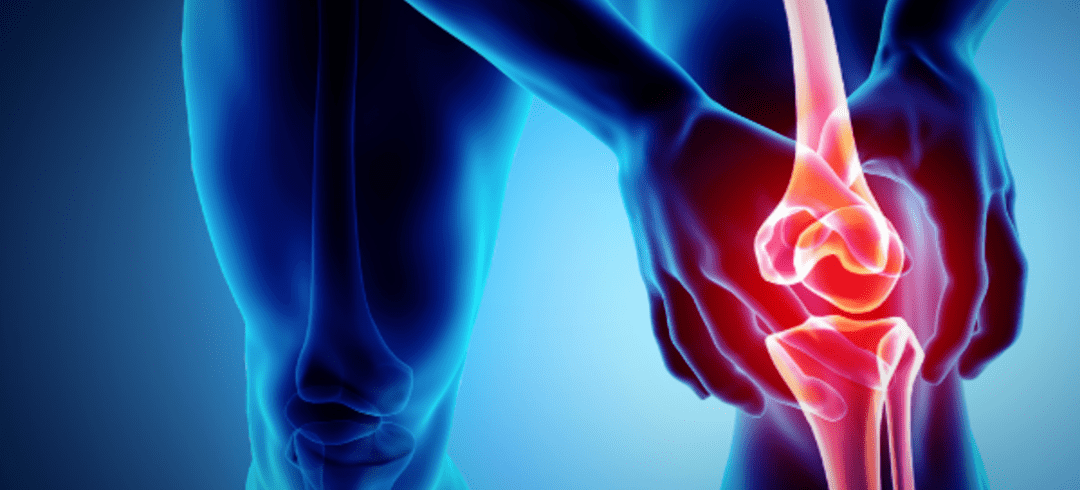
Stem cells are a groundbreaking form of regenerative medicine that is being used to potentially help manage many ailments, including orthopedic injuries and chronic conditions. This treatment option offers many potential benefits to patients that suffer from orthopedic conditions. Here we will talk about the Orthopedic benefits of Stem Cell Therapy.
While stem cell therapy is not necessarily a cure for these ailments, patients have reported improvements in their symptoms without the need for more invasive treatments such as surgery.
What is Stem Cell Therapy?
Stem cells are unique because they have the ability to divide and transform into specialized cells. Stem cells can facilitate the body’s natural healing processes and repair damaged tissue. However, the concentration of stem cells in your body naturally decreases as you age.
Mesenchymal stem cells can be harvested stem cells from one of several sources. Stem cells can be harvested from bone marrow aspirate, adipose (fat) tissue, or umbilical cords (Wharton’s Jelly). Once harvested, the stem cells are administered directly to the problematic areas and/or systemically with an IV.
Stem cell therapy targets your orthopedic ailment with a high concentration of these cells. These cells will divide and replace damaged tissue, thereby alleviating or improving your chronic orthopedic symptoms.
How Are Stem Cells Used to Treat Orthopedic Conditions?
Orthopedic conditions are usually the result of inflammation and damage to bone, ligaments, tendons, or cartilage. Stem cells are naturally drawn towards inflammation within your body. In addition, stem cells can differentiate into various cells, including progenitor cells. Once this occurs, they can transform into specialized cells, such as those in your musculoskeletal tissues.
Instead of managing orthopedic conditions with medication or surgical intervention, stem cells can offer an alternative option for patients to explore. These cells have the potential to provide the body the resources it needs to rebuild damaged tissues naturally.
Potential Benefits of Stem Cells
Stem cell therapy is continuing to be researched but studies have shown it to be a safe and potentially effective treatment option for many patients that are struggling with orthopedic conditions. While your physician cannot guarantee that your stem cell therapy will produce a specific outcome, this treatment option does offer many potential benefits.
Stem cell therapy uses natural materials and your body’s innate healing abilities to treat orthopedic conditions. This allows you the opportunity to manage your condition without the use of medications and surgical interventions. Many medications can have some side effects. Stem cells have been shown to have minimal side effects and are safe to be considered a natural option.
If you are struggling with chronic pain due to an orthopedic condition or injury, stem cell therapy may be a considered treatment option to potentially help manage symptoms and improve your daily quality of life. If you would like to learn more about the Orthopedic benefits of stem cell therapy contact a care coordinator today!
Don’t let pain control your life, call us at (800) 531-0831

by Stemedix | Aug 16, 2021 | Degenerative Disc Disease, Stem Cell Therapy
Degenerative disc disease is one of the leading causes of neck and low back pain in adults. This medical condition results in many symptoms. It is caused by wear and tear on the spinal discs. In this article, we are going to talk about Stem Cell treatment of Degenerative Disc Disease.
Aside from back and neck aches, degenerative disc disease can result in:
- Numbness
- Hot or shooting pains
- Weakness
- A “giving out” sensation
- Muscle spasms and tension
- And more
The most common symptom of this condition is constant and low-level pain. Chronic pain can make it difficult to live a normal life. Because of the discomfort that comes from degenerative disc disease, researchers are looking for innovative treatments to help patients live more comfortably.
Recent Phase III Trial Results for Stem Cell Therapies
A recent randomized Phase III trial has shown that stem cell injections can help patients with degenerative disc disease. According to the study, a single injection provided long-term relief of back pain. The study was conducted using stem cell products from Mesoblast Limited, an Australian regenerative medicine provider.
Representatives from the company hope to meet with the Food and Drug Administration (FDA) to speed up the approval of their product. The product in question is known as “remestemcel-L.” The company has been developing this stem cell product for several years.
Like many stem cell treatments, the product is made using bone marrow to harvest mesenchymal stem cells. Those cells are then injected into patients’ bodies to reduce inflammation. The product inhibits the development of certain inflammatory substances. Decreased inflammation reduces the patient’s pain.
According to the trial report, sixty percent of the injected patients reported little to no pain after a year. After two years, 54% reported minimal or no discomfort. The injections provided the most pain relief for patients who were in the early stages of the disease.
Reduced Use of Opioids
Studies like the one discussed above have given many patients and medical professionals confidence in the potential of stem cells. In the study by Mesoblast Limited, more than 400 volunteers participated. Many of the patients who experienced pain relief decreased their use of opioids. Across the study group, opioid use declined by 40%.
Patients in the control group who received a saline injection actually increased their use of opioids. Because of this, the company hopes that the FDA will fast-track the approval of remestemcel-L as a standard treatment for degenerative disc disease.
Future studies will be necessary to determine the full potential of stem cell therapies. Still, many patients have experienced significant improvements in their health and wellbeing by using stem cell therapies. If you are interested in using stem cell treatment for Degenerative Disc Disease contact a care coordinator today to learn more!

by Stemedix | Aug 9, 2021 | Multiple Sclerosis, Stem Cell Therapy
In the United States, nearly one million people suffer from multiple sclerosis (MS). That is nearly one in 330 people nationwide. While the condition is not exceedingly common, it also cannot be classified as rare. The current number of people who have MS has doubled which is why more researchers have been delving into ways to treat the condition. For MS, the mean age of patients at the time of diagnosis is 34 years. The vast majority of patients are diagnosed between the ages of 20 and 50. However, MS has also been known to affect children and teenagers. In this article, we are going to talk about the stem cell transplant benefits for patients with MS.
The Slowing of Progression
Much of the research and medical development for MS have been focused on slowing the progression of the disease. There are currently several medications on the market that are geared toward doing just that. There has also been stem cell research done that has shown positive results.
While many drugs have succeeded in slowing the progression rate of MS, one important downside is the cost. Long-term use of these medications can affect a patient’s budget. If remission is gained, however, the patient can discontinue those drugs indefinitely.
One experiment involved patients from four countries, including the United States. All of the patients were given chemotherapy. Following this treatment, half were given drugs and the other half were administered stem cell therapy.
All patients that received the stem cell injections were clear from recurring symptoms after a year. Only six out of 52 had recurring symptoms after three years. The results of this experiment were released just a few years ago and have garnered the attention of researchers, as well as the desire for more trials.
Older Research
Stem cell therapy for the treatment of MS has been around for longer than most people realize. It began in the 1990s with hematopoietic stem cells, or HSC transplants, for patients that were not responding well to the conventional medications given at the time.
The method used for some of these trials was immunoablation. This is the process of partially destroying a faulty immune system and then replacing it with newer, healthier cells. Researchers have used it in further studies based on its early encouraging results. With this in mind, there may be hope on the horizon for the use of stem cells to achieve remission. If you are interested in scheduling a consultation contact a care coordinator today!

by admin | Aug 6, 2021 | Stem Cell Therapy, Mesenchymal Stem Cells, Stem Cell Research
It is estimated that over 126 million Americans, or nearly one in two adults, are affected with some form of musculoskeletal disorder, condition, or injury – a number comparable to the percentage of the population currently living with a chronic lung or heart condition[1].
While there are a number of treatment modalities proven to be effective for treating musculoskeletal disorders, conditions, and injuries, using stem cells appears to be among the most explored promising potential option of these methods.
With mesenchymal stem cells (MSCs) being the preferred source of stem cell, mostly because of their abundance (including sources such as bone, tendon, skin, and blood) and ability to differentiate to many different tissues, orthopedic surgeons have focused largely on MSC therapies for healing a number of specific orthopedic conditions, including the healing of fractures, regenerating articular cartilage in degenerative joints, healing ligaments or tendon injuries, and replacing degenerative vertebral discs.
The goal of the comprehensive literature review conducted by Akpancar et al. was to evaluate the most recent progress in stem cell procedures and current indications in the orthopedic clinical care setting.
Specifically, as part of this review, the authors found that therapeutic applications using stem cells, and MSCs in particular, allow the stem cells to be used as progenitor cells as a way to enhance the healing and repair process. The authors point out that while many sources of stem cells have been considered for use in orthopedic procedures, including bone marrow-derived MSCs (BM-MSCs), adipose-derived stem cells (AD-MSCs), synovial tissue-derived stem cells (ST-MSCs), peripheral blood-derived progenitor cells, and bone marrow concentrate, the optimal source of stem cells has yet to be determined.
In addition, Akpancar et al. while reviewing the orthopedic indication of stem cells on various musculoskeletal disorders, conditions, and injuries, found that in large part, stem cell therapy demonstrated positive results in improved healing in a variety of orthopedic indications, including major orthopedic bone-joint injuries, osteoarthritis-cartilage defects, ligament-tendon injuries, as well as other conditions.
Despite these findings, the authors also point out that while there have been large amounts of preclinical studies conducted and there continues to be increasing interest in performing additional studies on human subjects, the current findings gathered from preclinical studies are still preliminary. Considering this, the authors recommend additional research be conducted to evaluate the safety and efficacy of stem cells therapy in orthopedic surgery.
Source: (2016, August 16). The Current Perspectives of Stem Cell Therapy in Orthopedic Surgery. Retrieved from https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5253188/
[1] “One in two Americans have a musculoskeletal condition: New report ….” 1 Mar. 2016, https://www.sciencedaily.com/releases/2016/03/160301114116.htm.

by Stemedix | Aug 2, 2021 | Stem Cell Therapy
Arthritis is a common affliction. Seniors, in particular, tend to experience arthritis in their shoulders, although athletes may also be affected. The bones and muscles in the shoulder joints experience daily use throughout a person’s life. After many years of constant movement, the tissue in and around joints wears down. This can lead to shoulder arthritis. Traditional treatments for this condition require a long and difficult recovery process. Many patients are unable to engage in their normal routines and activities, due to arthritis shoulder pain. Fortunately, stem cells for shoulder arthritis may have the potential to effectively treat shoulder arthritis. Below, we will examine how this innovative approach has helped some patients heal and experience pain relief.
Types of Shoulder Arthritis
The human shoulder has more range of motion than any other joint on the body. Because of this, it often loses functionality as you age. Usually, this is due to everyday wear and tear.
Osteoarthritis is the most common form of shoulder arthritis. But it is not the only type that patients experience.
Other types of arthritis in the shoulder include:
- Rheumatoid arthritis, caused by underlying inflammation
- Post-traumatic arthritis triggered by prior shoulder injuries
- Rotator cuff tear arthropathy from a prior rotator cuff tear
These are only a few examples of the types of arthritis that may affect the shoulder joint as you age.
Regenerative Therapy and Stem Cells Could Help
Traditional medical treatments for shoulder arthritis include physical therapy and surgery. Many of these options are invasive and require a long recovery period.
However, stem cell therapy is a minimally invasive outpatient procedure that many patients are finding to be helpful. There is some evidence that stem cell therapies may decrease arthritis pain and encourage the growth of new tissues. Stem cell therapies are all-natural. That is because the stem cells used in the treatments come from adult stem cells.
They may be found in adipose (fat), bone marrow, or umbilical cord (Wharton’s Jelly) tissues. Some treatments may also include platelet-rich plasma (PRP) that is drawn from your blood.
These mesenchymal stem cells will then be administered to the problem area to help your body heal naturally. Once injected, the stem cells and/or PRP will encourage your body to engage in its natural healing functions. Growth factors in stem cells encourage the regeneration of tissue and decrease in inflammation.
No matter what type of arthritis a patient may be facing, stem cells for shoulder arthritis offer a promising option for patients to explore. Some patients may also explore additional modalities such as prolozone (ozone therapy with added vitamins) or peptides (amino acids) in their healing plans.

by admin | Jul 30, 2021 | Stem Cell Research, Multiple Sclerosis, Stem Cell Therapy
Typically understood to support hematopoiesis and to produce the cells of the mesodermal lineage, mesenchymal stem cells (MSCs) found in bone marrow, fat, and other tissues of the body, have recently been found to contain additional properties that include immunomodulator and neurotrophic effects.
Considering earlier studies that have demonstrated favorable effects of MSC treatments in a variety of conditions – including stroke, multiple sclerosis, multi-system atrophy, and amyotrophic lateral sclerosis, Petrou et al. performed this double-blind study as a way to evaluate the best way of administration and the safety and clinical efficacy of MSC transplantation – specifically in patients with active and progressive multiple sclerosis.
The response of the 48 patients with progressive multiple sclerosis and with displaying evidence of either clinical worsening or activity during the previous year in this study were evaluated after being treated intrathecally (IT) or intravenously (IV) with autologous MSCs or with sham injections. Having identified a critical and unmet need for treatment, the goal of Petrou et al.’s study was to examine the therapeutic efficacy of MSC transplantation in this specific population.
Over the course of this controlled clinical trial, participants were randomly assigned to three treatment groups and treated (either intrathecally or intravenously) with autologous MSCs or with sham injections. At the 6-month mark, the authors of this study retreated half of the patients in both the MSC-IT and MSC-IV groups with MSCs, while the remaining participants were treated with sham injections. The same process occurred with patients initially treated with sham injections; meaning that at the 6-month mark, half were either treated with MSC-IT or MSC-IV.
Prior to the start of this study, Petrou et al. established a number of primary and secondary endpoints. Predetermined primary endpoints of this study included: the safety of the MSC-IV and MSC-IT treatments and the difference among the three groups in relation to performance on the Expanded Disability Status Scale (EDSS) at 6- and 12-month intervals. Predetermined secondary endpoints included the difference between the sham-treated and MSC-IT or MSC-IV treated group in the number of relapses and the relapse rate, the number of MRI gadolinium-enhancing lesions, the annualized rate of change in the T2 lesion load on MRI, percent brain volume change, performance on a series of physical and cognitive functions, and the retinal nerve fiber layer thickness.
At the conclusion of this 14-month trial, the authors reported that the study demonstrated positive results in all predetermined primary endpoints. More specifically, throughout the course of this study, the authors discovered that significantly fewer patients experienced treatment failure in the MSC0IT and MSC-IV groups compared with those in the sham-treated group. Additionally, over the course of the following year, nearly 59% and 41% of patients treated with MSC-IT and MSC-IV exhibited no evidence of multiple sclerosis activity; this is compared with less than 10% of patients in the sham-treated group.
Significant improvements of those receiving MSC-IT treatment (compared to sham treatment) were also observed in the following: ambulation index, the sum of functional scores, 25-foot timed walk test, 9-hole peg tests, PASAT and OWAT/KAVE cognitive tests, and newer biomarkers, including retinal nerve fiber layer and motor network. The authors also report beneficial, but less significant effects were observed in the MSC-IV groups.
Although the authors report a number of limitations associated with this study, including a small number of patients in each group, the short duration of the study, and the crossover design of the study (which could have resulted in a “carry-over” effect from the first cycle of treatment), they also conclude that the clinically significant findings observed in patients with progressive multiple sclerosis who were previously unresponsive to traditional or conventional therapies provide clear evidence of short-term efficacy and possible indications of neuroprotection induced by administration of autologous MSCs in patients with progressive multiple sclerosis.
In addition, the authors found that intrathecal administration of MSCs appears more beneficial than intravenous, as well as the potential benefits provided by receiving repeated injections of MSCs.
As such, Petrou et al. conclude by calling for a larger phase III study to confirm these findings and as a way to further evaluate the therapeutic potential of autologous MSCs in neuroinflammatory and neurodegenerative diseases, including active progressive multiple sclerosis.
Source: (2020, December 1). Beneficial effects of autologous mesenchymal stem cell … – PubMed. from https://pubmed.ncbi.nlm.nih.gov/33253391/


 St. Petersburg, Florida
St. Petersburg, Florida
