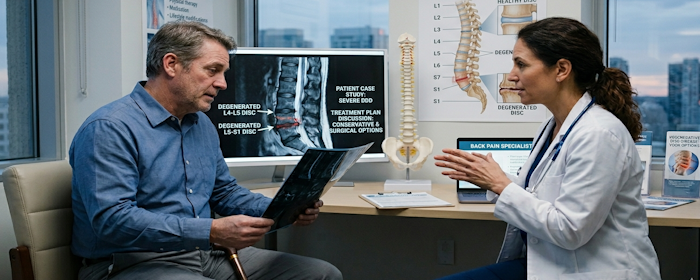
Regenerative Medicine for Degenerative Disc Disease: A New Approach to Chronic Low Back Pain
Low back pain is one of the most common health problems worldwide and a leading cause of disability. Most people will experience it at some point in their lives, and for many, it becomes a chronic condition that affects daily activities, work, and overall quality of life. One of the main underlying causes of chronic…