Traumatic Brain Injury Recovery: The Role of Regenerative Therapy in Improving Cognitive and Physical Function
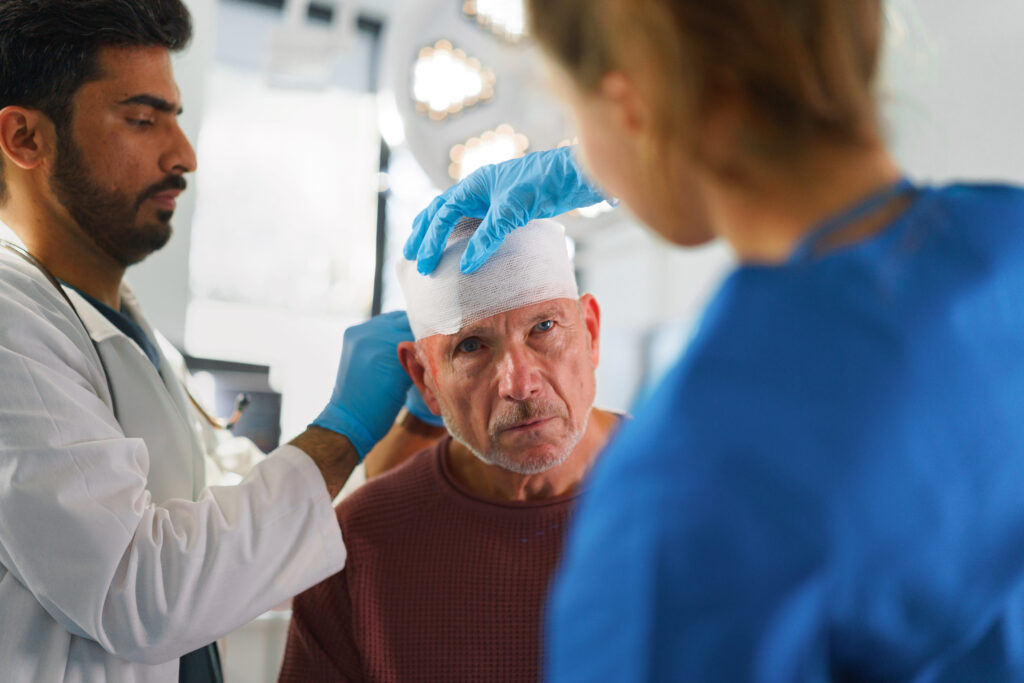
Traumatic brain injury (TBI) can create lasting challenges that affect your daily life, from memory lapses and reduced focus to difficulties with coordination and energy. At Stemedix, we focus on providing support through regenerative approaches that may help address the wide range of symptoms of TBI. Our team works with you to develop personalized therapy…