Diabetes Relief
Get Your Life Back with Diabetes Relief
Restoring Health to People with Metabolic Disease, Targeting the worldwide Diabetes Epidemic
Most Expensive Condition in the U.S.
$327 Billion: Total costs of diagnosed diabetes in the United States in 2017
$98 Billion spent on Diabetic Hospital Admissions
$10.9 Billion spent on Diabetic Neuropathy
1 in 4 Health Care $s incurred by Diabetics
NEW! Now accepting Medicare
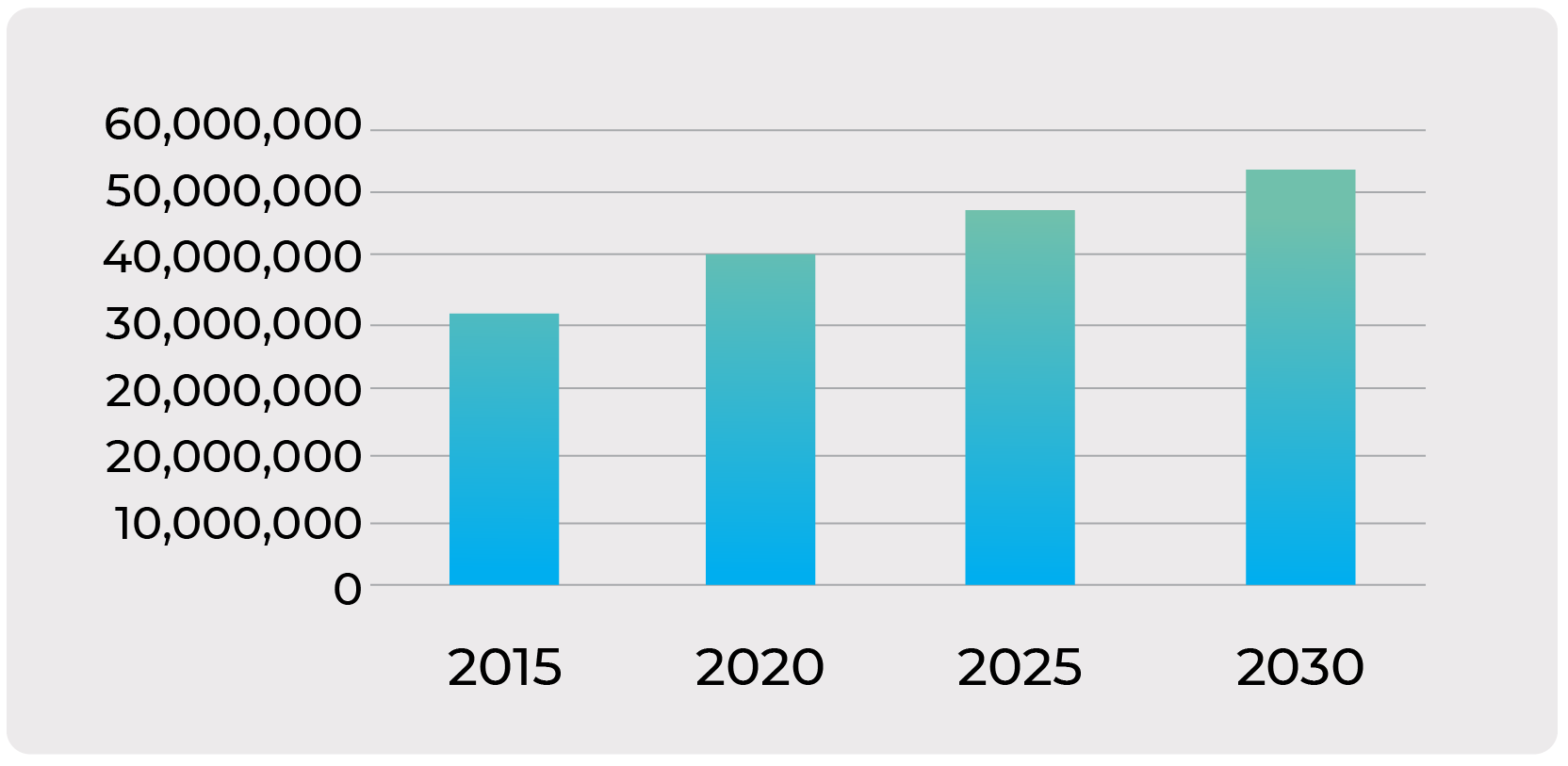
The Cost of Diabetic Care Will Increase 90% from 2015-2030
- Prevelance of Diabetes in the US will increase 54% during the same time period
- $622 Billion: Total annual medicaland societal costs will increase by 90%
- Dramatic Increased Costs as a result of diabetics living longer
Impact of Diabetes:
- Cardiovascular disease
- Nerve damage (neuropathy)
- Kidney failure (nephropathy)
- Eye damage (retinopathy)
- Foot damage (wounds & amputations)
- Skin conditions
- Hearing impairment
- Alzheimer’s (type 3 diabetes)
- Depression
- Stroke
- Peripheral Artery Disease
- Fatty Liver
- Gastroparesis
- Obesity
The Problem
Conventual methods focus on Symptom Suppression vs. addressing the root problem, Metabolic Failure
- The goal of these methods has never been to reverse the symptoms−only to delay them
- These methods have steadily increased healthcare costs
- Excessive Insulin: exposure is “toxic” resulting in insulin resistance and leads to diabetic complications
The Solution
- Physiologic Insulin Sensitization: naturally restores metabolism, improves carbohydrate processing & patient outcomes
- Diabetes Relief’s patented approach addresses the root problem and produces superior patient outcomes by mimicking the body’s natural method of regulating insulin.
Physiologic Insulin Sensitization
Patented Approach
Insulin as a Hormone vs. a Drug
The key to what makes DR so unique is that we use insulin as a hormone rather than a drug.
Physiologic Administration
By delivering insulin in a manner that mimics the normal physiologic secretion, we up-regulate insulin receptor activity and reduce insulin resistance.
Insulin Sensitization
With improved insulin sensitivity, carbohydrates can more readily enter cells and be converted into ATP via oxidative phosphorylation. Increasing cellular energy allows damaged tissues and organs to grow, repair, and regenerate. Thus, our modality not only stabilizes, but in many instances can even reverse complications of diabetes.
Symptom Suppression vs. Symptom Elimination
Insulin has been used as a “drug” since 1922 to suppress symptoms of high blood sugar. Diabetes Relief uses insulin intravenously as a “hormone communicator” in a more physiologically identical way to the body’s way of maintaining an optimized metabolism. Every patient’s degree of insulin resistance and efficiency of carbohydrate metabolism levels is unique; so, we begin with a consultation to determine medical necessity and establish an individualized care plan.
Induction to Maintenance
Although each patient’s care plan is unique, a typical type 2 diabetic starts the “Induction Phase” with 2 infusions per week then reduces to 1 per week for approximately 10 weeks. The Maintenance Phase is focused on finding the balance between an optimized metabolism for
the patient and extending as much time as possible between treatments. Typically, our patients achieve 4-6 weeks between infusions while maintaining optimized metabolism and insulin sensitivity.
Restoring, Repairing, Regenerating, but Not a Cure
Unfortunately, metabolic impairment is a chronic disease. If patients stop therapy the improvements experienced from Diabetes Relief treatments will wane over time.
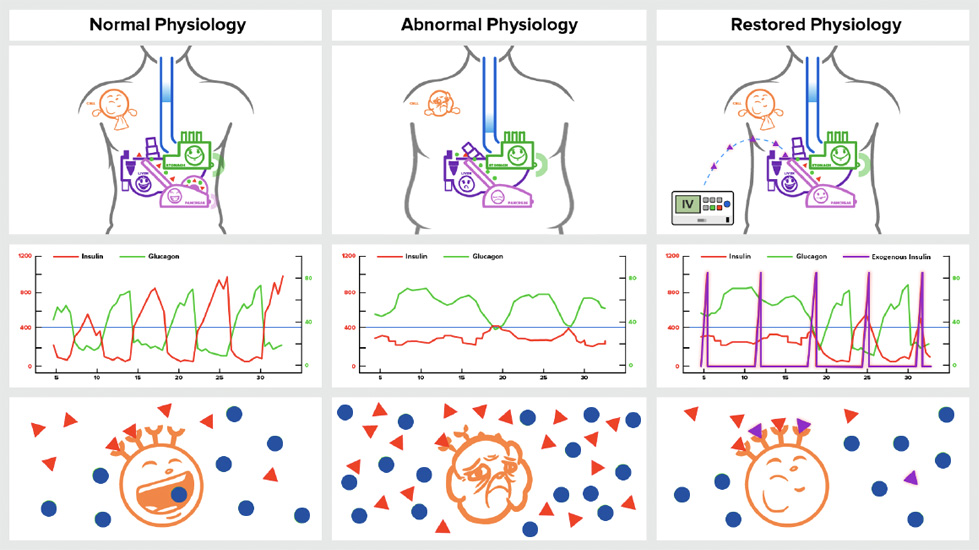
Mechanism of Action
The treatment is designed to reduce insulin resistance which is the primary cause of type 2 diabetic and many other metabolic disorders.
With improved insulin sensitivity at the insulin receptor level, glucose can more readily enter cells and be converted into adenosine triphosphate, also known as ATP –a molecule that carries energy within cells.
Through increasing cellular energy, the protocol is designed to repair and regenerate the body’s cells, peripherally at first, and then through repeated treatment sessions the cellular restoration progresses to the organ level which helps the body naturally return to more normal physiologic behavior.
Thus, the treatment has not only stabilized, but in many instances has reversed complications of diabetes and other metabolic disorders.
Treatment Overview
The treatment includes an intravenous precision administration of FDA approved fast acting insulin using an FDA approved portable pump.
The objective of the precise dosing is to achieve biomimicry of insulin as a hormone communicator to stimulate the metabolism –not to simply use insulin as a drug to suppress a high blood sugar which typically causes insulin resistance at the insulin receptor level.
The pumps patented biomimicry engineering combined with the treatment protocol are designed to administer insulin bioidentically to the body’s way of maintaining an optimized metabolism.
Along with the insulin hormone, the patient is given small specific amounts of glucose (ingested as a dextrose liquid) to stimulate and digestive systems and its role in the metabolism process during treatment.
Typical Care Plan
Every patient’s degree of insulin resistance and efficiency of carbohydrate metabolism is unique; so we begin with a consultation to determine medical necessity and establish a Physician Directed individualized care plan.
Each patient’s unique care plan typically includes an “Induction Phase” of 2 infusions per week reducing to 1 per week for approximately 90 days and a “Maintenance Phase” focused on finding the balance between an optimized metabolism and insulin sensitivity while extending as much time as possible between treatments.
Each treatment lasts approximately two to three hours, and the patient is free to move around the clinic during the treatment.
Typically, our Type 2 Diabetic, Prediabetic and Nondiabetic patients reduce from 3-hour infusions to 2-hour and achieve four to six weeks between infusions while maintaining optimized metabolism and insulin sensitivity.
Metabolic impairment is a chronic disease; therefore, if patients stop therapy the improvements experienced from treatments will diminish over time.

Frequently Asked Questions
-
–
What are the potential benefits?
While undergoing treatment over time, you will likely reduce some of the damage done by the diabetes and you may not need the same medication doses you did before the treatment. This could be the diabetes or non-diabetes medications.
If you have been on insulin for 3 or less years, it is highly likely that you will be able to get off insulin entirely. If you’ve been on it for >3 years, likely to be able to reduce it by 50%.
Who is a candidate?
Adults with type 1, type 2 DM, metabolic disorders, pre-DM, non-diabetics with or without complications (neuropathy, retinopathy, nephropathy, poor wound healing, ED, HTN, hyperlipidemia, obesity, fatty liver disease, stroke, Alzheimer’s, and/or Parkinson’s)
Who is NOT a candidate?
Pregnant or planning to be, patient on hemodialysis, unstable medical condition, unstable psychiatric patient, anorexia/eating disorder, bedridden/can’t come in and sit in chair or wheelchair, AND if NO LAB WORK DONE PRIOR.
What pre-treament labs are needed?
Patients need to have blood work done within 30 days of starting the treatment. Labs that are needed: CBC, CMP, fasting lipid panel, Hgb-A1C, c-peptide, insulin, Magnesium, vitamin D, Urinalysis with microanalysis, urine microalbumin, and potentially CRP, IL-6, TNF alpha, and BHCG (pregnancy test).
Follow-up lab testing varies per care plan: T7 or T14 – labs every 90 days, T21 or higher – labs every 180 days.
What do I need to do pre-treatment?
There are medication adjustments that need to be made prior to coming in for the appointment.
• If AM appt, take 1/2 dose of insulin (if on it) & other DM meds the night before. No DM meds to be taken the morning of the appointment.
• If PM appt, take normal dose of insulin (if on it) the night before, and take 1/2 dose of insulin and other DM meds the morning of the appointment.
• If on an insulin pump, turn it off 2 hours pre-treatment and turn on immediately post-treatment.
• For patients with Pre-DM or non-diabetic, they need to eat a high carb (healthy) meal prior to appt. Blood sugar should be >150 before starting treatment.
• If it’s lower, eat higher carb meal (oatmeal, pasta, or sweet potato).
• If it’s higher, eat fewer carbs and more protein meal (avocado with eggs, PB or almond butter with banana, salad with chicken or fish).


 St. Petersburg, Florida
St. Petersburg, Florida
