Extracellular Vesicle Therapy for Idiopathic Pulmonary Fibrosis: Mechanisms and Therapeutic Potential
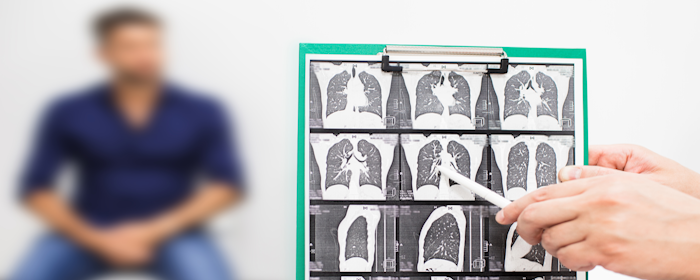
Idiopathic pulmonary fibrosis (IPF) is a serious and chronic lung disease marked by progressive scarring of lung tissue. Over time, this scarring thickens and stiffens the lungs, making it increasingly difficult for oxygen to pass into the bloodstream. As lung function declines, patients may experience shortness of breath, persistent dry cough, fatigue, and reduced exercise…