
by admin | Nov 5, 2018 | Hyperbaric Oxygen Therapy, Traumatic Brain Injury
Many US warfighters are left with traumatic brain injury (TBI) and/or posttraumatic stress disorder (PTSD) after suffering blast injury during battle. TBI is one of the leading causes of disability in the United States, and PTSD is rapidly becoming a leading cause of disability among US veterans. PTSD leaves sufferers with flashbacks, severe anxiety, sleep disturbances, mood disorders, and cognitive deficits. Traumatic brain injury, on the other hand, may cause a variety of mental and emotional problems. When these conditions occur in the same patient, it can have devastating effects on quality of life for the veteran’s remaining years.
The main treatment for traumatic brain injury is to simply allow the brain time to heal. Unfortunately, the brain is different than skin or other tissues of the body; it only has limited capacity to heal itself after an injury. The main treatment for PTSD is psychotherapy (talk therapy) and a rather nonspecific collection of medications including antidepressants and antipsychotic drugs. Unfortunately, people with both traumatic brain injury and PTSD are more difficult to treat, and generally, have poorer outcomes.
Researchers at the Veterans Administration studied the effects of hyperbaric oxygen therapy among military veterans with mild to moderate traumatic brain injury and PTSD. In a phase 1 clinical trial, veterans received 40 treatments of hyperbaric oxygen therapy lasting for 60 minutes each. Each treatment was 1.5 times atmospheric pressure or 50% more than they would experience under normal circumstances. Despite this modest dose of hyperbaric oxygen, the benefits to warfighters were remarkable.
After treatment, the veterans had substantial improvements in short-term memory, attention, concentration, and executive function. Shockingly, their IQ increased by nearly 15 points on average. They also enjoyed a substantial reduction in the frequency and severity of headaches. On average, they had a 30% reduction in PTSD symptoms. In fact, nearly 2/3 of trial participants were able to reduce the dose of or stop their PTSD medications.
Study participants also underwent special studies to examine the effects of hyperbaric oxygen therapy on brain tissue and blood flow. Patients treated with hyperbaric oxygen showed substantial increases in brain blood flow and marked increases in the volume of brain tissue. In other words, hyperbaric oxygen therapy was able to accelerate brain healing in this study.
This groundbreaking research has led to the use of hyperbaric oxygen therapy is a treatment for TBI and PTSD in other military personnel and also civilians. As additional clinical trials are published, the hope is that more health insurers, Medicare, and the VA will reimburse patients for this important treatment.

by admin | Sep 5, 2018 | Hyperbaric Oxygen Therapy, Stem Cell Research, Stem Cell Therapy, Studies, Traumatic Brain Injury
Traumatic brain injury (TBI) is one of the most common causes of disability in the United States, affecting over 13 million citizens. Traumatic brain injury is responsible for over 2 million emergency department visits, over a quarter of 1 million hospitalizations, and nearly 60,000 deaths each year.
Traumatic brain injury harms brain tissue in two phases. The first phase of injury occurs at the time of the traumatic incident. This initial injury may cause small or large areas of the brain to bleed. It may also shear (stretch/tear) nerve cells, making them dysfunctional. The second phase occurs hours or days after the initial injury. The brain is subjected to ongoing damage because of inflammation, cell death, and injury to blood vessels. Many people with TBI are left with lifelong problems with thinking, memory, and behavior.
In both of these phases of injury, one major way to help prevent long-term brain damage is by maintaining adequate blood flow to brain tissue. Unfortunately, once the damage has occurred, it can be a challenge to reverse the damage. Patients usually must endure months or years of physical and occupational therapy to regain what was lost. Moreover, patients often need substantial amounts of psychiatric and psychological support to treat mental health problems.
Fortunately, researchers are using hyperbaric oxygen therapy (HBOT) to improve blood flow to the brain in patients with traumatic brain injury. Hyperbaric oxygen therapy provides patients with pure oxygen (100%) at slightly higher pressures than they would experience normally. It is been used for hundreds of years to treat scuba divers who suffered “the bends” or decompression sickness; however, researchers are finding that hyperbaric oxygen therapy is a “coveted neurotherapeutic method for brain repair.”
To study the effects of hyperbaric oxygen therapy, researchers selected 10 people who had suffered mild traumatic brain injury in the previous 7 to 13 years. Patients all had brain damage that interfered with attention, memory, and thinking abilities.
Even though patients had sustained traumatic brain injury and brain damage a decade earlier, hyperbaric oxygen therapy was able to improve blood flow in the brain. Likewise, the amount of blood detected within the brain significantly increased, suggesting that hyperbaric oxygen therapy actually caused blood vessels in the brain to grow and multiply. Just as impressively, patients with chronic brain damage performed better on tests of cognition (i.e. thinking). They were able to process information more quickly, they had better motor function, and they were able to take in and process information about the world around them more efficiently.
Because people with traumatic brain damage have limited treatment options to improve their situations, these results are incredibly exciting. This was a study on 10 patients and more studies on larger numbers are still needed to build on these findings. Nonetheless, these results are quite encouraging for people with traumatic brain injury and their loved ones.

by admin | Aug 16, 2018 | Hyperbaric Oxygen Therapy, Bone Marrow, Stem Cell Research
Stem cells are generating so much excitement in research and clinical circles because they have the capacity to become many other types of cells. They also release a number of important molecules such as hormones, cytokines, and genetic material that can potentially be helpful for patients. Researchers have found that not only does hyperbaric oxygen therapy (HBOT) help in the circulation of stem cells but it also will help to mobilize stem cells from the bone marrow to the bloodstream further preparing the patient for stem cell therapy.
Bone marrow is a rich source of stem cells, but getting them usually requires an invasive procedure, i.e., placing a large bore needle into the middle of bone(s). Researchers have discovered, however, that hyperbaric oxygen treatment causes stem cells from the bone marrow to move into the bloodstream by specifically stimulating the body’s nitric oxide synthesis. Thus, instead of using a needle to extract stem cells from the bone marrow, patients can potentially increase their own bone marrow stem cells by undergoing hyperbaric oxygen treatment.
Stephen Thom, MD, Ph.D. and co-researchers at the University of Pennsylvania showed that a single hyperbaric oxygen treatment could double the number of bone marrow stem cells in the blood. This means that the hyperbaric oxygen was “mobilizing” the stem cells to move from the bone marrow into the bloodstream to allow them to move into areas of the body that benefit from them. Moreover, when study subjects underwent 20 treatments of hyperbaric oxygen therapy over a few weeks, the number of bone marrow stem cells in the blood increased significantly by eightfold. This astonishing finding has been confirmed in subsequent experiments.
The most important conclusion from this research is that hyperbaric oxygen therapy treatments can unlock the potential of a person’s own bone marrow stem cells without an invasive procedure. While many scientists assumed that the benefits of hyperbaric oxygen therapy were due to the high concentrations of oxygen infusing the blood, tissues, and cells, they now have research to support that these benefits may also be due to stem cell mobilization.

by admin | Aug 2, 2018 | Hyperbaric Oxygen Therapy, Stem Cell Research, Stem Cell Therapy, Studies
While most approaches to stem therapy involve infusing purified stem cells into the body, Thom and fellow researchers have shown that hyperbaric oxygen therapy (HBOT) is capable of stimulating the body to produce its own stem cells. Thom, Heyboer, and co-authors have extended this work by showing that by slightly increasing the pressures used during hyperbaric oxygen therapy, one can significantly increase the number of stem cells produced.
In his original work, Thom and colleagues showed that a single, two-hour session of 2.0 atmospheres (atm) pressure (twice the air pressure we normally feel at sea level) was capable of doubling the number of stem cells in the bloodstream. Twenty treatments increased stem cell levels by 800%. To study this phenomenon more closely, Thom’s research group recruited 20 patients to undergo hyperbaric oxygen treatment, some at the original 2.0 atm pressure, and some at 2.5 atm. The primary goal of this research was to find out whether a higher pressure was capable of eliciting a greater number of cells.
As before, treatment with 2.0 atm of hyperbaric oxygen substantially increased the number of stem cells found in the blood. However, treatment with 2.5 atm doubled or even tripled the number of stem cells produced compared to the 2.0 atm treatment session. In other words, a slightly higher pressure causes the body to produce substantially more of its own stem cells.
Researchers focused on two types of stem cells, in particular, CD34+ and CD45-dim—markers that appear on stem cells and/or progenitor cells. They are primarily found on cells in the bone marrow. Stem cells with CD45-dim generally go on to become bone, blood, or blood vessel cells, while CD34+ cells can differentiate into almost any cell. Hyperbaric oxygen therapy is thought to stimulate the bone marrow to produce and release these stem cells into the bloodstream, which is the reason these treatments raise stem cell levels in the blood.
The results published by Thom and coworkers suggest that patients who wish to enhance the number of stem cells should consider undergoing hyperbaric oxygen therapy. Furthermore, the greatest number of stem cells was observed after 20 treatment sessions, suggesting that a greater effect occurs with more treatments.

by admin | Jul 13, 2018 | Hyperbaric Oxygen Therapy, Stem Cell Therapy
Chronic fatigue syndrome, also known as systemic exertion intolerance disease, is a challenging condition for many patients, their families, and the doctors who care for them. The illness is difficult to diagnose since not all symptoms will appear in every patient. Some do experience feeling chronically fatigued yet may not have chronic fatigue syndrome.
Most patients with chronic fatigue syndrome have a sudden onset of fatigue that may occur soon after an infection, such as a cold, pneumonia, or mononucleosis. Patients with chronic fatigue syndrome usually experience overwhelming fatigue that may interfere with sleep and the ability to think and concentrate. Symptoms tend to get worse after periods of heavy physical activity, but may also occur after simply rising from a seated position or standing for a long period. Importantly, most patients with chronic fatigue syndrome began life with few or no symptoms. Many were previously high functioning in their daily lives who are now impacted by the symptoms they experience.
Just as chronic fatigue syndrome is difficult to diagnose, it is also difficult to treat. Not every treatment will work for every patient. In fact, there is no widely accepted, specific treatment for chronic fatigue syndrome. Treatment is mostly supportive and aimed at reducing symptoms. While many medications have been tried such as antidepressants, steroids, stimulants, vitamin B12, essential fatty acids (and many others), no drug treatment has been consistently successful at helping people with chronic fatigue syndrome.
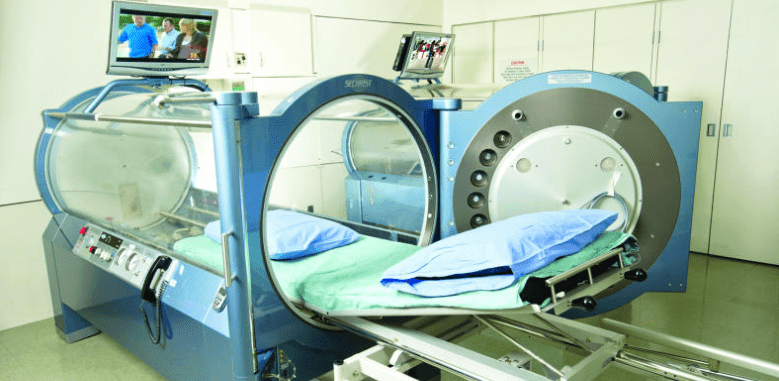
A recent report by Akarsu and colleagues may offer some hope for people with chronic fatigue syndrome. Sixteen patients with confirmed chronic fatigue syndrome received 15 sessions of hyperbaric oxygen therapy over a period of three weeks. Each treatment was for 90 minutes in a hyperbaric oxygen chamber. Participants in the study agreed to stop all physical therapy or medication for chronic fatigue syndrome so that those treatments would not interfere with the results of the study.
The research group found that chronic fatigue syndrome patients tolerated hyperbaric oxygen therapy very well, and had no complications. In all measures tested, patients were significantly better after treatment than they were before hyperbaric oxygen therapy started. Specifically, patients had better scores on two clinical tests of fatigue (visual analog fatigue scale and the Fatigue Severity Scale) and in a quality of life assessment (Fatigue Quality of Life Score). The improvement in scores was not subtle—in each test, there was a clinically significant increase in the average score. The results showed that hyperbaric oxygen therapy significantly and substantially reduced fatigue and improved quality of life in patients with chronic fatigue syndrome/systemic exertion intolerance disease. These results are incredibly encouraging since they indicate hyperbaric oxygen therapy may be an effective treatment for those battling chronic fatigue syndrome.



 St. Petersburg, Florida
St. Petersburg, Florida
