
by admin | Jul 5, 2019 | Stem Cell Therapy
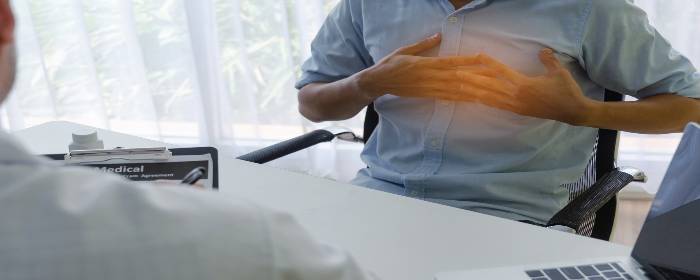
A heart attack is a life-threatening event in which blood flow through a coronary artery—and blood flow to the heart muscle itself—stops. If that blood flow is not quickly restored, heart muscle dies. A heart attack can be deadly if the heart is too badly damaged.
If someone experiences a heart attack, the heart muscle may be permanently weakened. Instead of having heart muscle that contracts to pump blood, the damaged heart tissue becomes full of fibers (fibrotic tissue) and is basically useless.
Regenerative Medicine has allowed scientists to reconsider whether this fibrotic tissue is permanently lost. Can stem cells prevent this fibrotic tissue from developing? Can new, healthy heart muscle be formed in its place? Recent research offers some tantalizing clues.
Researchers set out to determine whether mesenchymal stem cells taken from human umbilical cord could protect heart muscle cells (cardiomyocytes) after a heart attack. Specifically, the researchers were interested in learning whether exosomes collected from those stem cells (rather than the stem cells themselves) could protect cardiomyocytes.
To test this hypothesis, they created a heart attack in laboratory rats and administered exosomes they had gathered from mesenchymal stem cells. These particular mesenchymal stem cells were collected from human umbilical cord samples—the tissue that is normally thrown away after a baby is born.
The results of these experiments were interesting for several reasons. First, stem cell exosomes tipped the balance between fibrotic tissue (fibroblasts) and heart tissue (myofibroblasts). In other words, after an experimental heart attack, exosomes caused the heart to regrow more normal tissue than diseased tissue. Second, exosomes decreased the inflammation that occurs after a heart attack. It is believed that inflammation makes a heart attack worse. Lastly and perhaps most importantly, exosomes protected cardiomyocytes (heart muscle cells) from dying (through apoptosis).
Taken together, these results suggest that exosomes collected from umbilical cord mesenchymal stem cells protect heart muscle cells from the damaging effects of a heart attack in at least three important ways.
As these are early in Regenerative Medicine research, it is important to note that these experiments were performed in rats, and not humans. Interestingly, though, the stem cells were taken from human umbilical cords, and they were able to achieve these impressive effects in a different species (rodents). Obviously clinical trials are needed to determine whether this effect is applicable in humans; however, studies that use whole stem cells from human umbilical cord strongly suggest scientists are on the right track.
Reference: Shi, Y. et al. (2017). Exosomes Derived from Human Umbilical Cord Mesenchymal Stem Cells Promote Fibroblast-to-Myofibroblast Differentiation in Inflammatory Environments and Benefit Cardioprotective Effects. Stem Cells and Development. 2019 Jun 15;28(12):799-811.

by admin | Jun 27, 2019 | Stem Cell Therapy, Umbilical Stem Cell
Psoriatic arthritis is a chronic inflammatory condition that can become profoundly disabling. As a form of arthritis, the condition causes swollen, painful joints. The number and types of joints affected can vary over time, but most patients have polyarthritis i.e. arthritis in more than one body joint. Psoriatic arthritis also causes debilitating inflammation of the tendons, typically in the hands. Making matters worse, patients with psoriatic arthritis also suffer from skin rashes, eye problems, kidney and gastrointestinal problems, and profound fatigue. About one in five patients with psoriatic arthritis eventually develop severe manifestations of the disease in which the joints become permanently deformed and the surrounding bone breaks down.
The treatment of psoriatic arthritis usually includes a combination of drug and non-drug treatments. Nondrug treatments for psoriatic arthritis include exercise, physical therapy, and weight loss. Mild psoriatic arthritis is usually treated with nonsteroidal anti-inflammatory drugs such as naproxen. Moderate to severe psoriatic arthritis generally requires disease modifying anti-rheumatic drugs (DMARDs), which can include biologic and non-biologic agents. The typical non-biologic treatment for psoriatic arthritis is methotrexate. With the exception of severe disease, most physicians try methotrexate before using a biologic DMARD. If methotrexate fails, patients usually must move to one of the biologic agents, antibodies that are injected under the skin. Unfortunately, all DMARDs are associated with certain and sometimes severe side effects, and not every DMARD works for every patient with psoriatic arthritis.
Because psoriatic arthritis is potentially disabling and often difficult to treat effectively, researchers are aggressively pursuing other treatments. Stem cells offer a unique opportunity to provide patients with cells that can regenerate damaged joints and reverse the signs and symptoms of arthritis. To this end, Margaret Coutts and colleagues harvested stem cells from umbilical cord samples—the tissue that is routinely corrected after newborns are delivered is usually discarded as medical waste. They selected a patient with severe psoriatic arthritis would fail to find relief after nonsteroidal anti-inflammatory drugs, methotrexate, and biologic DMARDs. The researchers purified stem cells from cord blood and administered 200,000 cells per day to the 56-year-old man over a period of five days.
Within one week of umbilical cord stem cell treatment, the patient reported fewer and less severe psoriatic skin plaques and less joint pain. Encouraged by these results, the psoriatic arthritis patient continued receiving three rounds of stem cell treatments over six months. At the end of these treatments, the psoriatic skin plaques were almost completely gone, and the ones that remained were smaller, less prominent, and lost their red, scaly appearance. The man had substantially less joint pain and swelling and reported feeling “higher energy levels” and greater physical functioning. Lastly, laboratory markers of inflammation including ESR and CRP were noticeably improved.
Since these dramatic improvements occurred for only one person, they should be evaluated with caution. Additional studies with larger numbers of people are needed to make definitive conclusions. Nevertheless, umbilical cord stem cells led to profound improvements in this psoriatic arthritis patient’s life, a result that cannot be overstated.
Reference: Coutts, M. et al. (2017). Umbilical cord blood stem cell treatment for a patient with psoriatic arthritis. World Journal of Stem Cells. 2017 Dec 26; 9(12): 235–240.

by admin | May 30, 2019 | Lupus, Mesenchymal Stem Cells, Stem Cell Research, Stem Cell Therapy, Umbilical Stem Cell
Systemic lupus erythematosus or simply “lupus” is a chronic inflammatory disease that can affect almost every organ and tissue in the body. Most people are aware of chronic fatigue, muscle and joint pain, and a characteristic facial skin rash that occurs in people with lupus. However, the disease can affect the gastrointestinal tract, lungs, heart, eyes, lymph nodes, and brain. About half of all people with lupus will develop problems in their kidneys related to the disease. The most common kidney problem caused by lupus is a condition known as lupus nephritis.
Lupus nephritis may not cause any outward symptoms, though some patients report foamy urine. Physicians usually detect lupus nephritis during routine urinalysis. Lupus nephritis causes the kidneys to leak substantial amounts of protein in the urine. Over time, this protein loss can cause swelling in the hands, ankles, and feet, and may interfere with kidney function.
The main way in which lupus nephritis is treated is by using strong immunosuppressants such as glucocorticoids (“steroids”; prednisone), cyclophosphamide or mycophenolate mofetil. These immunosuppressing drugs can cause a number of serious and perhaps permanent side effects. Making matters worse, some people with lupus continue to have worsening lupus nephritis even after using these immunosuppressive drugs. In these cases, there is very little that can be done to treat the disease.
In order to help this group of individuals for whom regular treatments did not stop lupus nephritis from progressing, researchers conducted a clinical trial to test the effect of stem cells on this illness. Researchers collected allogeneic mesenchymal stem cells from bone marrow and umbilical cord tissue. They then infused the stem cells in 81 patients with lupus nephritis and followed them for 12 months. Amazingly, 60.5% of patients enjoyed remission of their kidney disease by the 12-month visit. Kidney function (glomerular filtration rate; GFR) significantly improved in patients treated with mesenchymal stem cells. Likewise, total lupus disease activity (not just lupus nephritis) improved significantly 12 months after treatment. These improvements were so profound that patients were able to reduce their doses of prednisone and other immune-suppressing drugs. Importantly, the stem cells did not cause any apparent adverse effects.
If this work can be confirmed in subsequent clinical trials, it is exciting news for patients with lupus, especially those with lupus nephritis. This work suggests that stem cells may be able to reduce the doses of immunosuppressants currently used to treat lupus nephritis, and it may even stop the progression of this terrible illness in some patients. We eagerly await additional clinical research in this area.
Reference: Gu F et al. (2014). Allogeneic mesenchymal stem cell transplantation for lupus nephritis patients refractory to conventional therapy. Clinical Rheumatology. 2014 Nov;33(11):1611-9.

by admin | May 22, 2019 | Bone Marrow, Mesenchymal Stem Cells, Stem Cell Research, Stem Cell Therapy, Umbilical Stem Cell
Mesenchymal stem cells have two unique and powerful properties that make them the focus of intense scientific research. First, mesenchymal stem cells can escape recognition by the immune system. In other words, when mesenchymal stem cells are infused into the body, the immune system does not recognize them as foreign and does not react to them. If the immune system did respond to the stem cells, it would cause an aggressive and potentially deadly allergic or immunologic response. Second, mesenchymal stem cells have the power to inhibit the immune system. This means mesenchymal stem cells could be used to treat immunological and autoimmune diseases such as Rheumatoid Arthritis, Systemic Lupus Erythematosus, Multiple Sclerosis, and Crohn’s Disease, among others. In essence, mesenchymal stem cells can affect the immune system without triggering an inflammatory response making them an ideal treatment for these diseases.
For some time, mesenchymal stem cells extracted from bone marrow were thought to be the only type of mesenchymal stem cells capable of beneficially affecting the immune system. This fact is not necessarily bad, but it does mean that mesenchymal stem cell donors must undergo a bone marrow procedure, which can be painful and expensive. It would be far better if doctors could use mesenchymal stem cells taken from easier-to-get tissues such as fat (adipose), umbilical cord blood, or Wharton’s jelly (umbilical cord tissue). Most people have adequate amounts of fat just under the skin, and umbilical cord blood and tissue are thrown away as medical waste every day.
Fortunately for patients, Dr. Yoo and colleagues showed that mesenchymal stem cells taken from fat tissue, umbilical cord blood, and Wharton’s jelly exhibit the same immunomodulatory properties as mesenchymal stem cells taken from bone marrow. The researchers showed that these types of mesenchymal stem cells were able to suppress T-cell proliferation as effectively as those cells taken from bone marrow. T-cell proliferation, it should be pointed out, is a key step in autoimmune inflammation that occurs in diseases such as rheumatoid arthritis and others.
In short, mesenchymal stem cells taken from easier-to-get tissues were just as effective at suppressing inflammation (in vitro) as those taken from bone marrow. These results will need to be confirmed in clinical studies; however, this approach will be much more convenient and less expensive for patients and donors if they can use mesenchymal stem cells taken from fat or umbilical cord rather than bone marrow and yet reap the same benefits.
Reference: Yoo KH et al. (2009). Comparison of immunomodulatory properties of mesenchymal stem cells derived from adult human tissues. Cell Immunology. 2009;259(2):150-6.

by admin | May 16, 2019 | Mesenchymal Stem Cells, Multiple Sclerosis, Stem Cell Research, Stem Cell Therapy
A new study has shown that a protocol for treating Multiple Sclerosis with stem cells is safe. According to the researchers, the potential for using stem cells in Multiple Sclerosis therapy warrants further investigation. The results of the study were published in the Journal of Translational Medicine.
Stem cells – and specifically, mesenchymal stem cells, have been increasingly used in the treatment of immune and inflammatory conditions. Based on the success that has been seen in these areas, scientists reasoned that mesenchymal stem cells may also represent a useful approach to treat Multiple Sclerosis, a neurological disease that involves the abnormal attack by the immune system on the myelin sheath that insulates nerves and allows nerve cells to communicate effectively and efficiently with one another.
To test this idea, the scientists used umbilical cord mesenchymal stem cells in 20 Multiple Sclerosis patients. The patients were given intravenous injections of the stem cells each day for seven days. The researchers evaluated the patients – with both neurological testing and nervous system imaging – at baseline, one month after treatment, and one year after treatment. The researchers found that the stem cell treatment improved neurological scores in patients and that lesions in the brain and cervical spinal cord were inactive one year after the stem cell injections. There were no serious adverse side effects associated with the treatment.
Based on these findings, it is possible that stem cells will provide a useful treatment option for those with Multiple Sclerosis. With more research, we will better understand exactly how stem cells can be used to help this population of patients.
Reference: Riordan, N.H. et al. (2018). Clinical feasibility of umbilical cord tissue-derived mesenchymal stem cells in the treatment of multiple sclerosis. Journal of Translational Medicine, 16(57), 1-12.

by admin | May 13, 2019 | Mesenchymal Stem Cells, Stem Cell Research, Stem Cell Therapy
Erectile dysfunction is the most common sexual disorder among men. During an erection, blood enters the tissues within the penis and is temporarily trapped there. In erectile dysfunction, however, this process does not occur. A man who suffers from this condition is unable to achieve a penile erection sufficient for sexual intercourse.
Erectile dysfunction has many causes ranging from neurological conditions to vascular (blood vessel) conditions to psychological conditions. In most men, erectile dysfunction is caused by a problem in blood flow and nitric oxide production, which is why drugs like the Viagra and Cialis are effective for some men because they temporarily reverse these problems.
Results from a review of 54 research studies showed that stem cell-based therapies may be able to reverse these effects on a more permanent basis. For example, mesenchymal stem cells were able to increase the number of enzymes that produce nitric oxide. Likewise, mesenchymal stem cells increased the size of penile tissue in older rats. Indeed, stem cell injections were able to restore erectile function in rats with diabetes.
Based on these laboratory results, researchers have conducted clinical trials using stem cells to treat men with erectile dysfunction. In one such trial, researchers used a person’s own fatty tissue (adipose) to generate stem cells. They then injected those cells into men with erectile dysfunction. Eight out of 11 men treated with stem cells regained erectile function. In another small study, eight men with profound erectile dysfunction in whom oral ED treatments failed received placenta-derived stem cells. Two of the patients were able to achieve and sustain erections six weeks after treatment while an additional patient was able to do so after three months.
Laboratory studies of stem cells in the treatment of erectile dysfunction are extremely promising. The clinical studies in this area are limited, and the results are somewhat less impressive. Nonetheless, as improvements and refinements are made to stem cell technology, this approach could offer hope to men with erectile dysfunction, especially those men who have not been helped by ED drugs.
Reference: Albersen, M. et al. (2013). Stem-cell therapy for erectile dysfunction. Arab Journal of Urology. 2013 Sep; 11(3): 237–244.




 St. Petersburg, Florida
St. Petersburg, Florida
