

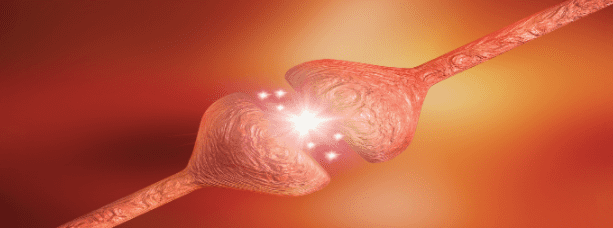
Stem Cell Therapy for Multiple Sclerosis and Neural Damage
Multiple sclerosis (MS) is an autoimmune disease that’s increasing in prevalence over the past few decades. According to the National MS Society, more than one million people live with multiple sclerosis in the United States alone. Globally speaking, MS is diagnosed in around 2.3 million patients, with hundreds of new cases every week. Interestingly, people who live in the Northern or Southern extremes of the planet are at a higher risk to develop MS than their counterparts.
Unfortunately, MS is a chronic, progressive condition with no curative treatment.
Multiple Sclerosis and its Impact on Brain Cells
The pathophysiology of MS is quite complex and involves the auto-destruction of the central nervous system (CNS) tissue by antibodies and immune cells. The main target of the immune reaction is the myelin sheaths found on neurons to facilitate electrical conduction. Unfortunately, those myelin sheaths also provide protection for neurons to maintain their optimal function.
Additionally, the inflammation mediated by the immune system damages the integrity of neurons, leading to the loss of millions of cells that play a crucial role in the function of the CNS. Another frustrating aspect of this malady is the recurrent relapses, where patients experience vision problems, muscular weakness, reduction in mobility, and balance issues even with adequate pharmacological therapy.
Today, there is one treatment option that is considered an alternative option to one’s journey to wellness and improvement of symptoms – stem cell therapy.
Stem cell therapy and Neural Damage
Mesenchymal stem cells (MSCs) have incredible regenerative and repairing properties due to their multipotent characteristic that allows them to differentiate into different body tissues. MSCs can be obtained from adipose tissue, bone marrow, umbilical cord (Wharton’s Jelly), and placenta.
For many years, researchers conducted studies to see if MSCs benefit patients with multiple sclerosis, and many results showed positive benefits.
For instance, in a 2019 study published by Stem Cell Investigation, researchers stated that “Upon intravenous injection, MSCs are able to traffic into the brain lesions and improve the survival rate of brain cells.” Although scientists are still researching the underlying mechanism that led to these results, the positive effects of MSCs are attributed to their regenerative, self-renewal, and immunomodulating properties.
One of the most appealing type of stem cell therapy is the umbilical cord-extracted MSCs because of the site’s accessibility, their potentcy, and the absence of any ethical issues. Overall, the scientific community believes that MSCs have great potential in the treatment of Multiple Sclerosis and other neurodegenerative conditions.
Stem cell therapy research has increased over the past few years and is making impacts in the history of medicine and biology. The regenerative properties of these cells has opened a new chapter in the management of conditions and their symptoms that can impact a person’s day to day life. Contact us today for a free consultation.
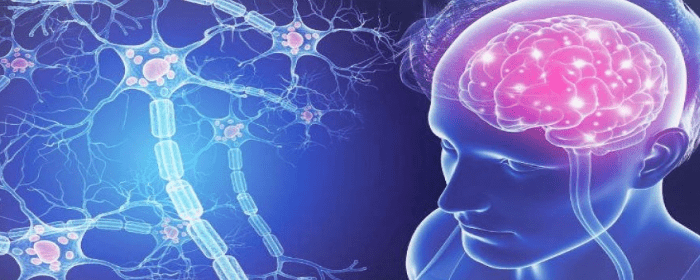
What Is Stem Cell Therapy for Multiple Sclerosis?
Multiple sclerosis (MS) is a condition that affects the central nervous system, disrupting the ways in which information flows within and to and from the brain. Its cause is unknown, though experts believe it may result from a combination of genetic and environmental factors. The trajectory and symptoms of the disease are often unpredictable. People with MS may experience symptoms related to movement, such as tremors or unsteady gait, as well as vision-related changes, slurred speech, tingling or numbness, and fatigue.
MS symptoms typically begin to emerge between the ages of 20 and 50. For some individuals, symptoms may improve or go into remission for periods of time. In some cases, MS symptoms can interfere with daily life, making it difficult to complete everyday activities.
While there are currently no cures available for MS, there are some medications available to aid in symptom management. Yet, these can be costly and may carry side effects.
Stem Cell Therapy for Multiple Sclerosis
Recently, stem cell therapy for Multiple Sclerosis has emerged as a promising treatment with tremendous potential. It is not a cure but has shown potential for symptom improvements. Mesenchymal stem cells (MSCs) have the ability to help control inflammation and restore the myelin sheath, the protective covering that surrounds nerve fibers which is damaged in MS. These powerful cells also have the ability to regulate the immune system, which can aid in symptom reduction.
The reason the immune regulating effects of MSCs are so beneficial to people with MS is that they prevent the immune system from mistakenly attacking the myelin sheath. MSCs may even regenerate myelin sheath where it’s been damaged, known as remyelination.
While results may vary, MS patients who receive stem cell therapy may experience a number of benefits. Some reported include increased energy, strength, mobility, flexibility, and function control. The treatment is also noninvasive, well-tolerated in most patients, and does not require any downtime. With its lasting beneficial healing properties, stem cell therapy appears to be an alternative option, especially for patients whose symptoms interfere with daily life.
If these beneficial healing properties are something you would like to take advantage of then contact us today for a free consultation.
How Exosomes Can Improve Stem Cell Therapy
Given the limitations of several conventional methods to treat a wide variety of diseases and injuries, stem cell therapy has begun to gain in popularity. The evidence supporting the field of Regenerative Medicine, which involves using stem cells to regenerate healthy, functional tissue, has indeed been accumulating in recent years.
There are a number of different types of stem cells that have been explored for their therapeutic potential. Mesenchymal stem cells have become a preferred option for therapy because of their ability to differentiate into several different types of adult tissue and to be transplanted safely and effectively into patients.
One-way mesenchymal stem cells confer their therapeutic benefits is through paracrine effects that are achieved by the secretion of extracellular vesicles, some of which are exosomes. Exosomes are between 30 and 100 nanometers (nms) in diameter and exist in blood, cerebrospinal fluid, and other bodily fluids.
A recent review, published in Cell Transplantation, covered research showing that mesenchymal stem cell exosomes are therapeutically advantageous for the management of several conditions, including Parkinson’s disease, osteoarthritis, and stroke.
The review discusses, for instance how in models of Parkinson’s disease, exosomes have been shown to provide neuroprotection. MSC-derived exosomes also appear to inhibit inflammation in the context of osteoarthritis and also to stimulate repair in damaged tissue. Further, specific exosome biomarkers, miR-9 and miR-124, have proven to be promising in diagnosing the severity of stroke.
Based on recent research covered in this review, stem cell-derived exosomes have significant therapeutic potential. Though this review focuses specifically on the relevance of exosomes in Parkinson’s disease, osteoarthritis, and stroke, exosomes will likely provide benefits for patients in a variety of contexts and will prove to be an important part of Regenerative Medicine.
Reference
Chang, Y-H, et al. (2018). Exosomes and stem cells in degenerative disease diagnosis and therapy. Cell Transplantation, 27(3), 349-363.

 St. Petersburg, Florida
St. Petersburg, Florida
