
by Stemedix | Oct 19, 2020 | Stem Cell Therapy, Pain Management
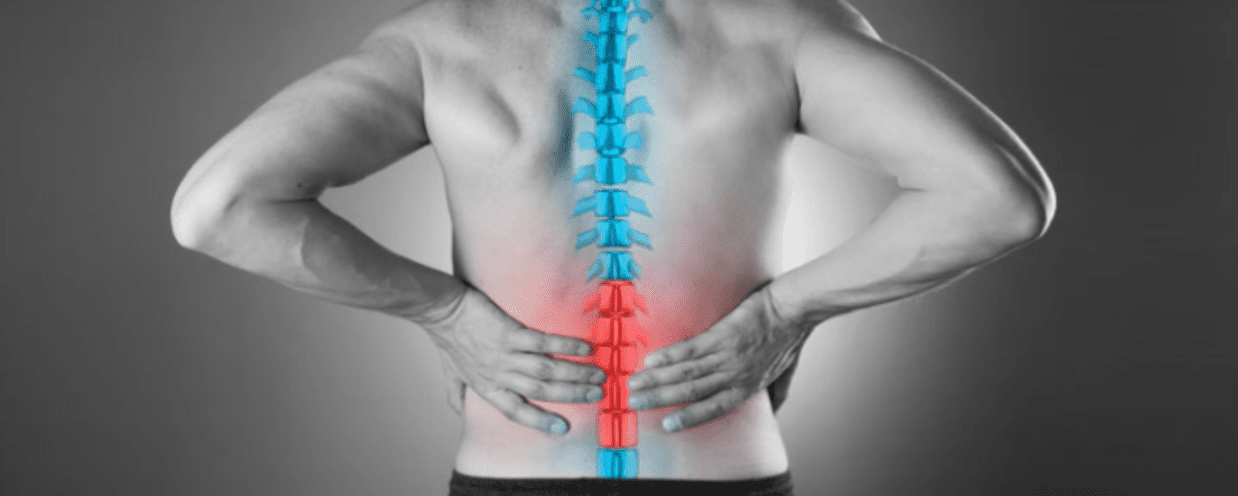
Half of all working adults in the U.S. report back pain symptoms each year. In many cases, the issue is acute and will resolve over time. In other cases, the pain can be pronounced and intensify if left unaddressed, interfering with daily activities. Understandably, many patients hope to avoid invasive back surgeries but are still seeking relief through other means. When conventional therapies fall short, stem cell therapy could be a solution for you.
Stem Cell Therapy as a Back-Pain Treatment
Existing treatments for many conditions causing pain in the back include anti-inflammatory and prescription pain medications, physical therapy, and lifestyle modifications. When pain is severe, more invasive approaches, including surgical spinal fusion, may be recommended. Unfortunately, pain can persist even after surgery.
Today, patients have an alternative minimally invasive option. Stem cell therapy is being leveraged to improve lower back pain to do some of the following:
- Repair disc or facet joint damage
- Improve function
- Alleviate chronic pain
The treatment has been implemented for a number of back conditions, including degenerative disc disease, spinal cord injury, herniated discs, sciatica, and spinal facet disease. The stem cells can be strategically administered with the goal of restoring structural integrity, function, and pain reduction.
With spinal facet disease, the stem cells can be directed to the cartilage surrounding the spinal facet joints to reduce pain and inflammation and improve mobility. The injection is performed via x-ray guidance for the utmost level of precision.
If you’re experiencing pain from disc or facet injuries caused by arthritis, overuse, or trauma, you could potentially be an ideal candidate for stem cell therapy for back pain. The treatment is widely considered to be safe and effective, and in addition to being minimally invasive, requires little recovery time before yielding improvements. Contact a Care Coordinator today for a free assessment!

by admin | Oct 16, 2020 | Alzheimer’s Disease, Stem Cell Research, Stem Cell Therapy
Alzheimer’s disease is the most common form of dementia. Among other symptoms, Alzheimer’s disease causes memory loss as nerve cells in the brain become dysfunctional and die. While the disease is known to be related to the accumulation of β-amyloid plaques and neurofibrillary tangles, how and why those things happen is still a mystery. Nonetheless, researchers have created and tested drugs to change the way the brain process β-amyloid and hyperphosphorylated tau (the substance in neurofibrillary tangles) but nothing, so far, has worked in humans. Instead, we are left with anticholinergic drugs, and memantine used to slow the progression of the disease.
These failures of drug development have forced scientists to reconsider how to treat Alzheimer’s disease. Instead of a focus on neuropathology that we cannot understand or control, why not focus on supporting nerve cells that remain or even restore the nerve cells that are lost? This is the hope of stem cell research in Alzheimer’s disease, and the focus of an extensive review article on the subject.
The review article describes the clinical possibilities of different types of stem cells:
- Neural stem cells (NSCs)
- Mesenchymal stem cells (MSCs)
- Induced pluripotent stem cells (iPSCs)
Neural stem cells (NSCs)
NSCs have the magnificent ability to become any type of brain cell, be they neurons or various types of glia. NSCs would be the ideal stem cell treatment for Alzheimer’s disease except for one major problem: There are very, very few NSCs in the human brain. It is nearly impossible to harvest them in high enough numbers and, right now, we don’t have ideal ways to make them multiply and grow in a laboratory. So, while research in NSCs for the treatment of Alzheimer’s disease is well underway, they won’t be widely available any time soon.
Mesenchymal stem cells (MSCs)
Mesenchymal stem cells can become many different types of cells and can be harvested from many places including bone marrow, umbilical cord, and adipose (fat). MSCs are very versatile, and we are improving at safely using them in various diseases, including Alzheimer’s disease. MSCs are one of the more exciting avenues of research in Alzheimer’s disease and other neurodegenerative diseases.
Induced pluripotent stem cells (iPSCs)
iPSCs are a remarkably interesting type of stem cell. They are stem cells that are created by reprogramming cells found in the skin (fibroblasts) to become other cells of interest. Researchers take fibroblasts and genetically alter them to behave like other types of stem cells or fully differentiated cells. Recent work has shown that scientists can repurpose iPSCs to become neural precursor colonies, which are a lot like NSCs described above. If one could take iPSCs from the skin and convert them into NSCs, this could truly be a treatment for Alzheimer’s disease.
Stem cell treatments provide the promising potential to help those with Alzheimer’s disease and other neurodegenerative diseases. While research is ongoing, the breakthroughs that have been recently discovered provide hope to those seeking an alternative option.
Reference: Lee, J. H., Oh, I. H., & Lim, H. K. (2016). Stem Cell Therapy: A Prospective Treatment for Alzheimer’s Disease. Psychiatry Investigation, 13(6), 583–589. https://doi.org/10.4306/pi.2016.13.6.583

by Stemedix | Oct 12, 2020 | COPD, Stem Cell Therapy
Chronic obstructive pulmonary disease (COPD) is a lung condition in which airflow to and from the lungs is obstructed, making it increasingly difficult to breathe. The World Health Organization estimates that the condition is the third-leading cause of mortality worldwide. There is currently no cure for COPD, although there is a COPD treatment available to help control its progression.
Recently, researchers have begun to study regenerative medicine approaches, which may be used to treat COPD and actually reverse some of the damage already done to the lungs. Stem cell therapy is one particularly promising option.
How Can Stem Cells Be Used as a COPD Treatment?
Stem cells act as the foundation for all cell types. They have the ability to proliferate and transform into adult cells and can repair injuries. They also have regenerative properties and can therefore help heal compromised lung tissue.
At the site of a wound, stem cells differentiate and release pro-inflammatory cytokines and growth factors to help draw healing proteins to the injury. Because the stem cells themselves are anti-inflammatory and anti-fibrosis (meaning they reduce the formation and build-up of scar tissue), they appear to be particularly useful for treating conditions, such as COPD.
How Are Patients Responding to Stem Cell Therapy for COPD?
While clinical trials and studies are still ongoing, stem cell therapy has provided patients with improvements in quality of life, such as improved energy levels, improved sleep quality, and reduction in the rate of tissue damage, and restoration of lung structure and function.
What Is the Process for Stem Cell Therapy for COPD?
Patients who are eligible candidates for stem cell therapy can either have stem cells retrieved from their own tissue, such as fat tissue or donated from umbilical cord tissue. The process is quick, simple, and painless. Stem cell therapy is well-tolerated in the majority of cases, is considered to be safe, and offers a potential alternative option for patients to consider. Contact a Care Coordinator today for a free assessment!

by admin | Oct 6, 2020 | ALS, Stem Cell Research, Stem Cell Therapy
ALS, which stands for amyotrophic lateral sclerosis, is a neurodegenerative disease that has no cure and no substantially effective treatment. Today, there are two drugs available that can slow the progression of ALS— riluzole and edaravone—but these agents may only be modestly effective. Sadly, patients with ALS get progressively worse, sometimes even with treatment. They lose to ability to move, to swallow, and to breathe. It is a devastating disease.
As with other neurodegenerative diseases, researchers are trying to treat ALS with stem cells. Stem cells have the capacity to become other types of cells such as neurons or glia. The notion is that stem cells could be used to rescue and replenish the nerve cells that are dysfunctional or destroyed in ALS. Studies are emerging that suggest that these approaches may bear fruit.
One such stem cell trial comes out of India, published by Dr. Prabhakar and colleagues. The research scientists infused autologous bone marrow-derived stem cells (autologous means the cells were retrieved from the patient and then readministered to the same patient). The scientists conducted the clinical study in ten patients with ALS who had a mean revised ALS Functional Rating Scale score of 30.2 ± 10.58. In other words, patients with this score have about a 60 to 70% chance of being alive for 9 more months.
Impressively, patients treated with autologous bone marrow-derived stem cells did not have a significant reduction in ALS Functional Rating Scale score after one year, which means their disease stayed relatively stable over this time instead of deteriorating. It took about 16.7 months for the score on this scale to drop by 4 points, which is considered a significant drop. The median survival after the procedure was 18.0 months, which is substantially more than would have been expected at the start of the study.
Taken together, these results suggest that patients with moderately severe ALS enjoyed a stabilization of their ALS symptoms for over 16 months on average. While there was no placebo control group, the stem cell-treated patients survived about twice as long as was estimated at the start of the trial.
These positive results must be confirmed in a larger, placebo-controlled trial. However, they strongly argue for further research of stem cells for the treatment of amyotrophic lateral sclerosis.
Reference: Prabhakar S, Marwaha N, Lal V, Sharma RR, Rajan R, Khandelwal N. Autologous bone marrow-derived stem cells in amyotrophic lateral sclerosis: A pilot study. Neurol India 2012;60:465-9

by admin | Sep 30, 2020 | Alzheimer’s Disease, Stem Cell Therapy
Alzheimer’s disease, the most common form of dementia, affects nearly 50 million people around the globe. That number is expected to more than double in the next 30 years without effective treatment. Currently, the treatments for dementia are only mildly effective. The few dementia medications that are available simply prolong the inevitable, slowing cognitive decline modestly.
Even with dementia medication, patients with Alzheimer’s disease and most other dementias have progressive memory loss. Over time they lose the ability to perform common everyday tasks. If patients live long enough, they will become dependent on others for all of their care. In this way, dementia is a devastating illness for loved ones.
Alzheimer’s disease and other dementias are neurodegenerative diseases, which means nerve cells in the brain become dysfunctional and die. As brain cells lose their ability to function, the person loses the abilities those nerve cells once performed. Since brain cells have little natural capacity to regenerate, once they are sick and die, that particular brain function may be lost forever.
Stem cells have long been an attractive potential option for Alzheimer’s disease and dementia treatment. Since brain cells become sick and die, the alternative option most recently looked at is to restore and replace those cells with stem cells—cells that can become brain cells? Indeed, stem cells may do so much more. They release countless molecules that help brain cells grow and survive. Not surprisingly, stem cells are the focus of intense research as a treatment for Alzheimer’s disease and other neurodegenerative diseases.
Drs. Duncan and Valenzuela reviewed the current status of stem cells as a possible treatment for Alzheimer’s disease and dementia. The research in animals has been incredibly promising. When stem cells are given to lab animals with experimental dementia, the stem cells find their way to the site of the disease and become new and healthy brain cells.
The research in animals has been so promising, that a number of Phase I and Phase II clinical trials in humans have been completed or are underway. From these trials, we know that stem cells appear to be safe for use in people with Alzheimer’s disease in that no serious adverse events were tied to stem cell use. It is too early to tell if these treatments will change the course of the disease until results are published. For now, we remain cautiously optimistic that the incredible effects of stem cells seen in animals may also translate to the same benefits in humans.
Reference: Duncan T, Valenzuela M. Alzheimer’s disease, dementia, and stem cell therapy. Stem Cell Res Ther. 2017;8(1):111. Published 2017 May 12. doi:10.1186/s13287-017-0567-5

by admin | Sep 25, 2020 | Autoimmune, Stem Cell Therapy
Humans cannot practically live without an immune system. The immune system helps us prevent and fight off infections and detect and destroy cancer cells. For some, however, experience conditions that affect the immune system. Autoimmune diseases such as multiple sclerosis, polymyositis, atopic dermatitis, and rheumatoid arthritis can make day to day activities challenging.
Patients who do not find relief from current therapies such as immunosuppressants and biologic agents, or those who cannot tolerate the side effects, are limited to optimal options. And when the autoimmune disease is severe, the patient’s quality of life is extremely low.
Researchers recruited patients with various, difficult-to-treat autoimmune diseases to study stem cell treatment outcomes. These patients had tried many other autoimmune disease treatments, and all had failed. The stem cell treatment used in these cases was called “compassionate use” since the patients had exhausted other treatment options and their conditions were all progressed. This compassionate use indication allowed researchers to use large numbers of stem cells—higher than are normally used in stem cell therapy.
The scientists took small amounts of stem cells from adipose tissue, i.e. fat tissue. Under laboratory conditions, they “expanded” the purified stem cells. In other words, the researchers took a relatively small number of stem cells and caused them to multiply them into millions of cells. Millions of cells were needed so that the doctors could have substantial treatment doses for each patient. The patients with autoimmune diseases received multiple doses of adipose-derived mesenchymal stem cells intravenously. These patients were then followed clinically to observe any change in their disease.
The first thing that the researchers noted was that high doses of stem cells did show to be safe. Multiple infusions of up to 1 billion stem cells infused over less than a month did not result in adverse events.
Just as importantly, people who had failed all other autoimmune disease treatments saw benefit from mesenchymal stem cell therapy. Patients with rheumatoid arthritis or polymyositis who could not stand or walk before treatment were showing success in standing and walking post-treatment. Patients with severe atopic dermatitis had substantial improvements in symptoms. Even a person with progressive autoimmune hearing loss had their hearing restored in one ear (and partially improved in the other ear) after mesenchymal stem cell therapy.
The astonishing results will need to be corroborated in a larger number of patients, but this study did reveal that high dose stem cells were safe in people with various autoimmune diseases. Those who do suffer from debilitating autoimmune diseases and who have not found relief from other treatments may want to research and consider stem cell therapy for a possible alternative option to help manage symptoms.
Reference: Chan Ra, J., et al. (2011). Stem cell treatment for patients with autoimmune disease by systemic infusion of culture-expanded autologous adipose tissue-derived mesenchymal stem cells. J Transl Med. 2011; 9: 181.


 St. Petersburg, Florida
St. Petersburg, Florida
