
by admin | Sep 5, 2018 | Hyperbaric Oxygen Therapy, Stem Cell Research, Stem Cell Therapy, Studies, Traumatic Brain Injury
Traumatic brain injury (TBI) is one of the most common causes of disability in the United States, affecting over 13 million citizens. Traumatic brain injury is responsible for over 2 million emergency department visits, over a quarter of 1 million hospitalizations, and nearly 60,000 deaths each year.
Traumatic brain injury harms brain tissue in two phases. The first phase of injury occurs at the time of the traumatic incident. This initial injury may cause small or large areas of the brain to bleed. It may also shear (stretch/tear) nerve cells, making them dysfunctional. The second phase occurs hours or days after the initial injury. The brain is subjected to ongoing damage because of inflammation, cell death, and injury to blood vessels. Many people with TBI are left with lifelong problems with thinking, memory, and behavior.
In both of these phases of injury, one major way to help prevent long-term brain damage is by maintaining adequate blood flow to brain tissue. Unfortunately, once the damage has occurred, it can be a challenge to reverse the damage. Patients usually must endure months or years of physical and occupational therapy to regain what was lost. Moreover, patients often need substantial amounts of psychiatric and psychological support to treat mental health problems.
Fortunately, researchers are using hyperbaric oxygen therapy (HBOT) to improve blood flow to the brain in patients with traumatic brain injury. Hyperbaric oxygen therapy provides patients with pure oxygen (100%) at slightly higher pressures than they would experience normally. It is been used for hundreds of years to treat scuba divers who suffered “the bends” or decompression sickness; however, researchers are finding that hyperbaric oxygen therapy is a “coveted neurotherapeutic method for brain repair.”
To study the effects of hyperbaric oxygen therapy, researchers selected 10 people who had suffered mild traumatic brain injury in the previous 7 to 13 years. Patients all had brain damage that interfered with attention, memory, and thinking abilities.
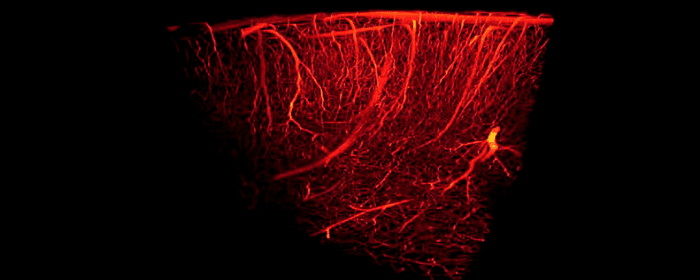
Even though patients had sustained traumatic brain injury and brain damage a decade earlier, hyperbaric oxygen therapy was able to improve blood flow in the brain. Likewise, the amount of blood detected within the brain significantly increased, suggesting that hyperbaric oxygen therapy actually caused blood vessels in the brain to grow and multiply. Just as impressively, patients with chronic brain damage performed better on tests of cognition (i.e. thinking). They were able to process information more quickly, they had better motor function, and they were able to take in and process information about the world around them more efficiently.
Because people with traumatic brain damage have limited treatment options to improve their situations, these results are incredibly exciting. This was a study on 10 patients and more studies on larger numbers are still needed to build on these findings. Nonetheless, these results are quite encouraging for people with traumatic brain injury and their loved ones.

by admin | Aug 31, 2018 | Stem Cell Research, Stem Cell Therapy, Studies
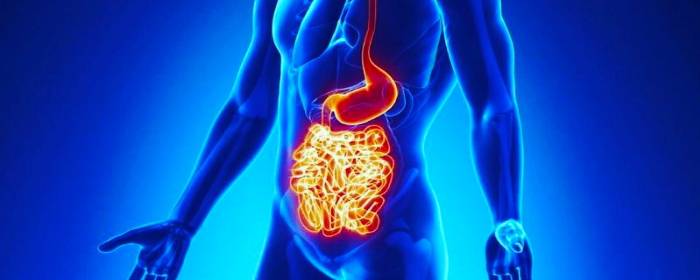
Crohn’s disease is a chronic inflammatory bowel disease that has no cure. It causes abdominal pain, frequent diarrhea, weight loss, fatigue, and anemia. While the disease can be controlled to some degree through oral and injectable medications, life-threatening complications may occur.
One of the feared complications of Crohn’s disease is called a bowel fistula. A fistula is an abnormal connection between two places on the body. In Crohn’s disease, a fistula forms between the intestine and some other structure—the intestine essentially forms a “tunnel.” The fistula can form between one loop of intestine and another, between intestine and bladder, or even between the intestine and the outside of the body. This complication of Crohn’s disease is obviously quite distressing to patients.
Some bowel fistulas may close on their own with conservative treatments, but fistulas associated with Crohn’s disease do not respond well to available medical treatments. Those looking for an alternative treatment may be able to consider stem cell therapy.
Stem cells offer an interesting potential solution to this problem. Stem cells can provide a large dose of normal cells filled with molecules that can help direct normal bowel growth and development. Indeed, researchers have shown that autologous mesenchymal stem cells can help close and heal fistulas in patients with Crohn’s disease.
In phase I, II, and IIB clinical trials, stem cells derived from adipose tissue or bone marrow were directly infused into the bowel area (via a so-called intra-fistular injection). Across five clinical studies including over 100 patients, stem cell administration resulted in complete fistula healing in 50 to 80% of patients treated. Of those who did not obtain complete control fistula closure, almost all had evidence of improvement. These results support that autologous mesenchymal stem cell therapy is a promising future treatment for patients with Crohn’s disease and may offer patients enjoy a better quality of life.

by admin | Aug 28, 2018 | Stem Cell Research, Stem Cell Therapy
The evidence for the promise of mesenchymal stem cells in regenerative medicine has been growing for several years. With new sources regularly emerging, stem cells can come from a large variety of sources. Postnatal mesenchymal stem cells appear to have the most promise in regeneration. A new review has addressed how mesenchymal stem cells can be used with innovative scaffolding engineering approaches to improve techniques in regenerative medicine.
Mesenchymal stem cells are, on their own, good candidates for regeneration because of a number of characteristic features. For instance, they can differentiate into many different types of cells. Osteoblasts and chondroblasts are two cell types that mesenchymal stem cells differentiate into and that can be supported in bone regeneration by 3D-printed biomaterials like scaffolds.
Mesenchymal stem cells also can have beneficial impacts on the immune system. Unlike with other stem cell types, the severe immune reactions that may occur with the transplantation of foreign materials into the body can often be avoided with the use of mesenchymal stem cells, making them a safe option in regenerative medicine.
The current review addresses the ways in which bone regeneration can be optimized through the use of mesenchymal stem cells and scaffold engineering and how new concepts in bioengineering may be able to improve regenerative medicine in combination with mesenchymal stem cell approaches. Future research will need to focus on how we can customize regenerative approaches using what we know about mesenchymal stem cells and the most cutting-edge innovations in bioengineering.

by admin | Aug 27, 2018 | Adipose, Stem Cell Research, Stem Cell Therapy
Regenerative medicine is a field of research concerned with the process of replacing diseased, dying, or dead cells with the intent of restoring structure and function. In its most basic form, regenerative medicine seeks to regrow cells that were lost or damaged due to injury or condition. Examples of regenerative medicine applications include restoring heart cells after a heart attack, repairing brain cells in Alzheimer’s disease or after stroke, or regenerating T-cells in HIV/AIDS. The potential applications of regenerative medicine are virtually limitless.
Adipose-derived stem cells hold great promise in the field of regenerative medicine. The stem cells are multipotent, which means they can become any number of cell types. For example, adipose-derived stem cells can become osteocytes (bone cells), neural cells (nerve cells), vascular endothelial cells (cells that make up blood vessels), cardiomyocytes (heart muscle cells), pancreatic β-cells (cells that produce insulin), and hepatocytes (liver cells).
Adipose- or fat-derived stem cells have one obvious advantage over bone marrow cells: they are much easier to obtain. Bone marrow stem cells require an uncomfortable/painful procedure to extract them from the center of the bone. Fat-derived stem cells, on the other hand, can be taken from fat pockets in any number of places just under the skin. This essentially combines a sort of liposuction with stem cell transplantation.
Adipose-derived stem cells are the subject of nearly 200 clinical trials worldwide. Even now, fat-derived stem cells are proving useful in several clinical conditions. Adipose-derived stem cells were shown to help people after they suffered from a heart attack, by reducing the size of the damaged heart and helping to restore heart function.
Another advantage of adipose-derived stem cells is that they present possess a tri-germ lineage differentiation potential, meaning they can differentiate into all three germ layers. In other words, they have the remarkable potential to become virtually any cell in the body. This means they can be applied to more than one disease state. In neurodegenerative diseases, such as post-stroke, adipose-derived stem cells could be used to create nerve cells (neurons) and the other main type of brain cell, called glia. Both cell types are destroyed during a stroke, and both are important for proper brain function.
As more results are published from dozens of clinical trials, we will get a clearer picture of the therapeutic potential of adipose-derived stem cells. Indeed, the future of regenerative medicine is very bright.

by admin | Aug 16, 2018 | Hyperbaric Oxygen Therapy, Bone Marrow, Stem Cell Research
Stem cells are generating so much excitement in research and clinical circles because they have the capacity to become many other types of cells. They also release a number of important molecules such as hormones, cytokines, and genetic material that can potentially be helpful for patients. Researchers have found that not only does hyperbaric oxygen therapy (HBOT) help in the circulation of stem cells but it also will help to mobilize stem cells from the bone marrow to the bloodstream further preparing the patient for stem cell therapy.
Bone marrow is a rich source of stem cells, but getting them usually requires an invasive procedure, i.e., placing a large bore needle into the middle of bone(s). Researchers have discovered, however, that hyperbaric oxygen treatment causes stem cells from the bone marrow to move into the bloodstream by specifically stimulating the body’s nitric oxide synthesis. Thus, instead of using a needle to extract stem cells from the bone marrow, patients can potentially increase their own bone marrow stem cells by undergoing hyperbaric oxygen treatment.
Stephen Thom, MD, Ph.D. and co-researchers at the University of Pennsylvania showed that a single hyperbaric oxygen treatment could double the number of bone marrow stem cells in the blood. This means that the hyperbaric oxygen was “mobilizing” the stem cells to move from the bone marrow into the bloodstream to allow them to move into areas of the body that benefit from them. Moreover, when study subjects underwent 20 treatments of hyperbaric oxygen therapy over a few weeks, the number of bone marrow stem cells in the blood increased significantly by eightfold. This astonishing finding has been confirmed in subsequent experiments.
The most important conclusion from this research is that hyperbaric oxygen therapy treatments can unlock the potential of a person’s own bone marrow stem cells without an invasive procedure. While many scientists assumed that the benefits of hyperbaric oxygen therapy were due to the high concentrations of oxygen infusing the blood, tissues, and cells, they now have research to support that these benefits may also be due to stem cell mobilization.

by admin | Aug 14, 2018 | Bone Marrow, Stem Cell Research
Colitis is inflammation of the colon, also known as the large intestine. Several things can cause colitis such as infection, medication, ischemia, or chronic inflammatory bowel disease. Inflammatory bowel diseases that affect the colon, such as ulcerative colitis or Crohn’s disease, are particularly challenging for patients. It is a chronic disease that causes cramping pain, bloody diarrhea, weight loss, fatigue, and many other chronic, challenging symptoms.
Since ulcerative colitis does not occur naturally in animals, researchers sometimes use an experimental form of colitis to mimic the disease seen in humans. This experimental colitis serves as a model to investigate treatments for inflammatory bowel disease. Essentially, researchers create a situation in which mice develop a condition that looks very much like ulcerative colitis. They develop inflammation in the large intestine, along with signs of oxidative stress and cell death. Conversely, treatments for ulcerative colitis reduce or prevent inflammation, oxidative stress, and cell death in the colon of these experimental mice.
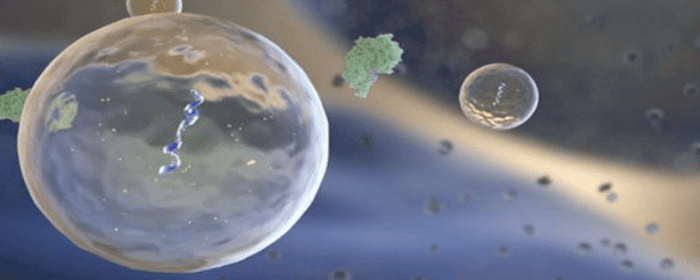
Researchers used this model of experimental colitis to study the effect of bone marrow stem cells as a treatment for colitis. More specifically, they tested the effects of a certain part of bone marrow stem cells called extracellular vesicles. Extracellular vesicles are small spheres that containing various beneficial substances. Stem cells release these vesicles into the body. A single stem cell can release hundreds of extracellular vesicles. In fact, it is the extracellular vesicles that are believed to contain many of the useful substances that are released by bone marrow stem cells such as proteins, lipids, and nucleic acids. These substances can precisely target sick and damaged cells in the body and repair them.
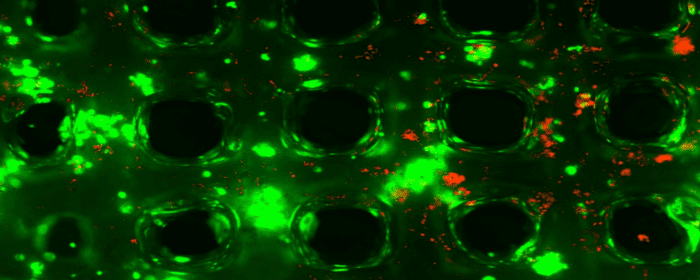
Impressively, when researchers used extracellular vesicles derived from bone marrow stem cells to treat animals with experimental colitis, they observed rather extraordinary results. These vesicles protected the intestines from colitis damage. Untreated animals had severely damaged intestines when viewed under a microscope, but animals treated with extracellular vesicles had nearly normal looking intestines. Treatment also substantially reduced levels of cytokines related to oxidative stress, such as IL-1β. Extracellular vesicles derived from bone marrow stem cells also apparently blocked the intestinal cells’ ability to undergo cell suicide (apoptosis).
Taken together, these results strongly suggest that mesenchymal stem cells from bone marrow, specifically the extracellular vesicles contained within them, can dramatically improve experimental colitis. While more research is needed, this study suggests that these stem cell products could one day be a useful treatment for inflammatory bowel diseases, such as ulcerative colitis and inflammatory bowel disease.



 St. Petersburg, Florida
St. Petersburg, Florida
